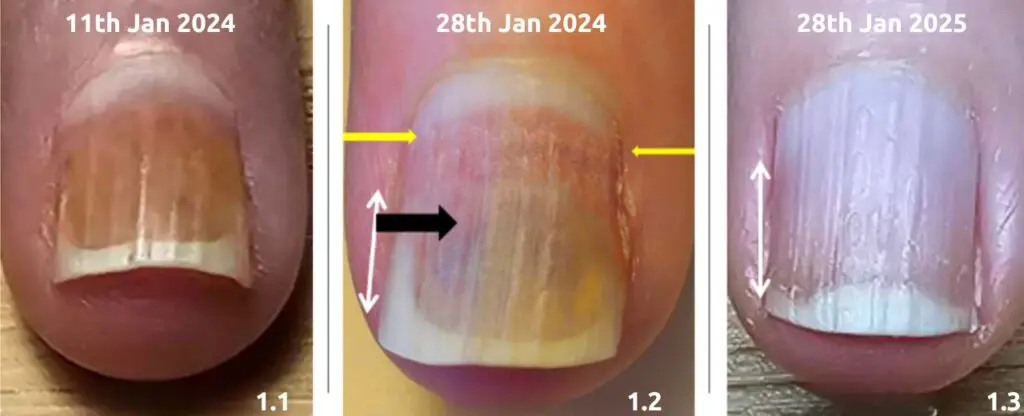
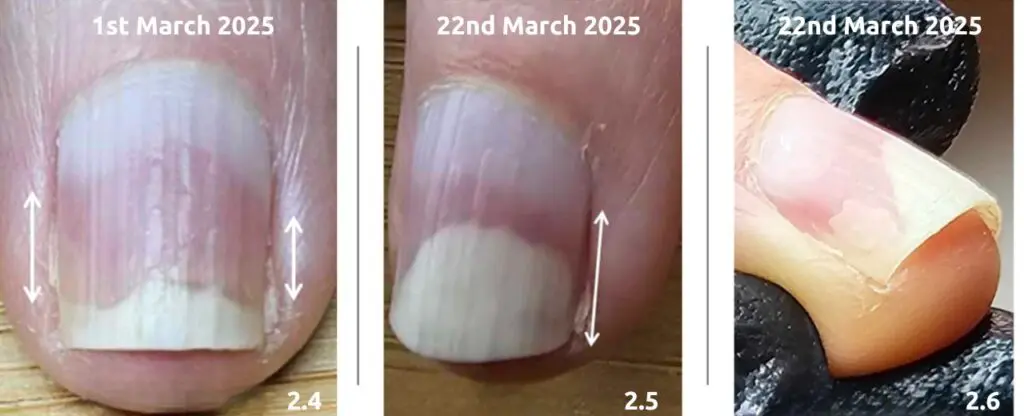
A real-world case of mixing nail brands and lamps
Mixing nail brands and lamps is a common temptation for professionals, especially when transitioning to new systems. One technician recently shared her story: despite strict hygiene standards and properly maintained lamps, she faced client issues such as lifting, splinter hemorrhages, and what appeared to be a fungal infection. Concerned that her products were to blame, she considered switching to a hypoallergenic brand but asked if she could safely keep her existing colours and top coat while using a new lamp and builder gel.
This raised a difficult question: could the products or the curing system be to blame? The technician began exploring the option of switching to a hypoallergenic brand but asked if it would be safe to use a new brand’s lamp and gel constructor while keeping her existing colours and top coat.
This scenario reflects a common dilemma in the nail industry, especially when transitioning between systems while managing costs.
Nail conditions linked to lifting and mixed systems
The word “fungus***” is often used by clients to describe any discolouration or problem under a nail, but true onychomycosis (fungal infection) develops slowly and is rarely caused by nail services alone. In many cases, what appears to be fungus is actually a bacterial issue such as Pseudomonas, sometimes called a “greenie.” This thrives in the space between the natural nail plate and lifted product.
***A fungal infection can be proved or ruled out using a test – it cannot be diagnosed by eye, even medical specialists or medical hand specialists can only suspect a fungal infection until proven otherwise.
**Bacterial infections could be a problem if your client is suffering from some kind of immune disorder or diabetes so be very careful and never ‘assume’
Lifting may be triggered by poor adhesion, trauma, over-filing, or incomplete curing. It is rarely the fault of the product alone. Recognising the difference is essential. Bacterial infections are managed differently from true fungal infection, which requires medical treatment.
Splinter hemorrhages and nail damage explained
Splinter hemorrhages are small streaks of blood beneath the nail plate. These are nearly always caused by trauma, but that does not necessarily mean one dramatic knock, repeated tapping, subtle pressure, or a nail coating that is overly rigid or unbalanced is the only reason, it can be an accumulation of more than one cause.
While these marks can worry clients, they are not usually caused by the products themselves. However, poor adhesion and repeated cycles of lifting and reapplication can make the nail plate more vulnerable to damage and by definition the nail bed more vulnerable.
Allergies and sensitivity from under-cured gels
Allergic contact dermatitis linked to nail products has been on the rise. Builder gels and hybrid products have come under scrutiny due to the frequency of reactions reported by both clients and professionals.
The key driver of these reactions is exposure to uncured or under-cured ingredients. Even when a coating looks hardened, if it has not cured completely, monomers remain present. These can penetrate the nail plate and irritate the surrounding skin, eventually leading to allergy. Once developed, an allergy to nail products is permanent.
A hypoallergenic system can reduce, but not remove, this risk. The greatest safeguard is correct curing and keeping all uncured product away from any and all living skin.
Why mixing nail brands and lamps is risky
Each professional gel system is designed, tested, and certified as a complete unit: capa base, builder or colour, top coat, and lamp. The lamp’s wavelength output, intensity, and cure time are matched precisely to the photoinitiators in that brand’s gel.
When technicians attempt to mix systems, for example by curing one brand’s colour coat under another brand’s lamp, there is no guarantee of complete cure. The coating may harden on the surface but remain only partially polymerised beneath. This is one of the leading causes of both service breakdown and allergic reactions.
According to NailKnowledge, nails cured under the wrong lamp may never fully cure, even after weeks. Filing or removing these coatings later releases uncured dust that can cause skin irritation and long-term sensitivity.
Phasing in a hypoallergenic system without mixing products
The financial reality is that not every professional can replace all products at once. However, trying to combine systems to save costs is not a safe solution. A smarter approach is to phase in a new hypoallergenic system gradually but keep each client service consistent.
That means if a client books for the hypoallergenic option, you use the same brand for base, builder, colour, top, and lamp. For other clients, you continue to use your existing full system. What you must avoid is cross-curing — using a lamp and builder from one system while keeping another brand’s colour or top coat.
This way you can manage costs while ensuring the safety of your clients and yourself.
The hidden danger of under-curing when mixing systems
One of the challenges is that under-curing is not always obvious. A nail may feel hard, look shiny, and even wear well, yet still contain uncured material beneath the surface. Over time, this hidden weakness can cause lifting, allow bacteria to grow in gaps, and expose both client and technician to sensitising dust during removal.
This explains why some issues are blamed on “bad product” when the real cause lies in mixing systems or using the wrong lamp.
Professional standards and insurance risks with mixed products
There is also a serious professional risk when dealing with clients who present with suspected infections or damage. If a client shows signs of bacterial or fungal involvement, the service should be stopped immediately and the client referred to a medical professional. Proceeding in such cases is not only unsafe but also invalidates insurance coverage.
Ignoring these guidelines can leave a professional personally liable if a client files a claim. Proper record-keeping and responsible referral protect both the client and the technician.
Key takeaways for nail Key lessons on mixing nail brands and lamps for professionals
- Nail infections and splinter hemorrhages often arise from lifting, trauma, or incomplete curing rather than product faults.
- Allergic reactions are increasing due to exposure to under-cured products. Once an allergy is developed, it is lifelong.
- Mixing nail brands and lamps introduces a significant risk of incomplete curing. This risk is invisible and accumulates over time.
- Transition to hypoallergenic systems should be phased in service-by-service, ensuring all products and the lamp are from the same brand for each client.
- Always refer clients with suspected infections to a medical professional before offering further services.
Conclusión
The temptation to mix systems is understandable, especially with financial pressures, but the evidence shows it is not safe. Lamps and gels are not interchangeable. The best course for nail professionals is to use each system as it was designed and to phase in new products as complete sets.
Client trust and long-term safety depend on professional standards, and cutting corners by mixing nail brands and lamps can lead to problems that are far more costly than any short-term savings.