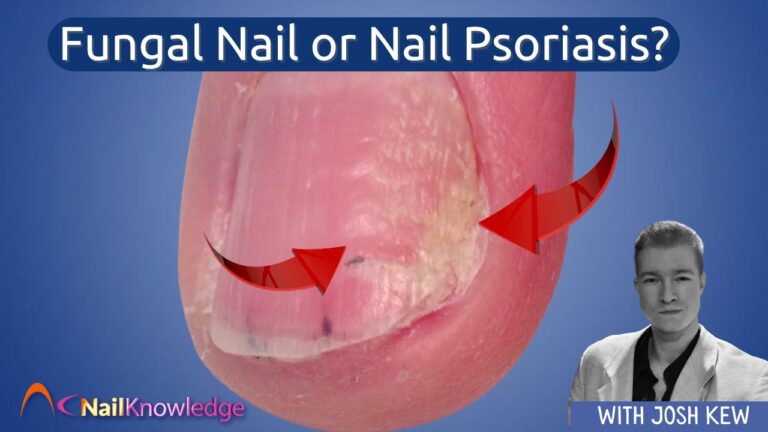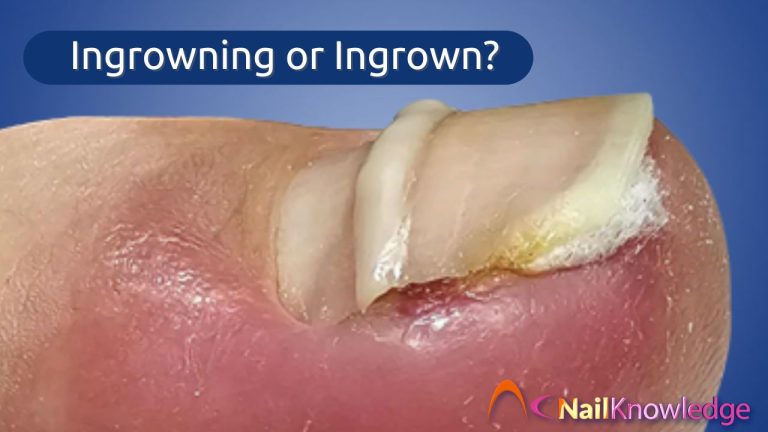
Unha encravada ou encravada no dedo do pé - Causas, sintomas e conselhos sobre cuidados
Understanding an Ingrowing vs Ingrown Toenail An ingrowing toenail occurs when the edge of the nail starts pressing into the surrounding skin. An ingrown toenail…
Read More →